Polycystic Ovary Syndrome (PCOS) is a hormonal condition that affects millions of women worldwide. From irregular periods and acne to insulin resistance, weight changes, and fertility concerns, PCOS impacts far more than just your reproductive system.
Because PCOS affects multiple systems in the body, managing it often requires care from more than one medical professional. This guide breaks down the doctors you should see if you have PCOS, what each specialist does, and how they support long-term health.
Gynecologist (OB-GYN): The First Doctor for PCOS

A gynecologist is usually the first doctor involved in diagnosing PCOS.
How a gynecologist helps with PCOS:
Diagnosing PCOS using symptoms, blood work, and ultrasound
Treating irregular, heavy, or absent periods
Managing ovarian cysts
Prescribing birth control or cycle-regulating medications
Addressing pelvic pain or abnormal bleeding
When to see a gynecologist:
If your periods are irregular, unpredictable, painful, or missing—or if you suspect PCOS—this should be your first step.
How an endocrinologist helps with PCOS:
PCOS is a hormonal and metabolic condition, making endocrinologists essential for deeper care.
Managing hormone imbalances (androgens, insulin, thyroid)
Treating insulin resistance or prediabetes
Supporting metabolic health and weight regulation
Monitoring long-term hormonal risks
When to see an endocrinologist:
If blood sugar issues, unexplained weight gain, or abnormal hormone levels are present—or if symptoms aren’t improving with basic treatment.
General Practitioner (GP): Your Long-Term Health Partner
Your primary care physician plays a crucial role in managing overall health with PCOS.
How a GP helps with PCOS:
Routine blood tests and health screenings
Monitoring cholesterol and blood pressure
Screening for type 2 diabetes and heart disease
Coordinating referrals to specialists
When to see a GP:
Regularly. PCOS increases long-term risks for cardiovascular and metabolic conditions, making ongoing monitoring essential.
Dermatologist: Treating PCOS Skin and Hair Symptoms
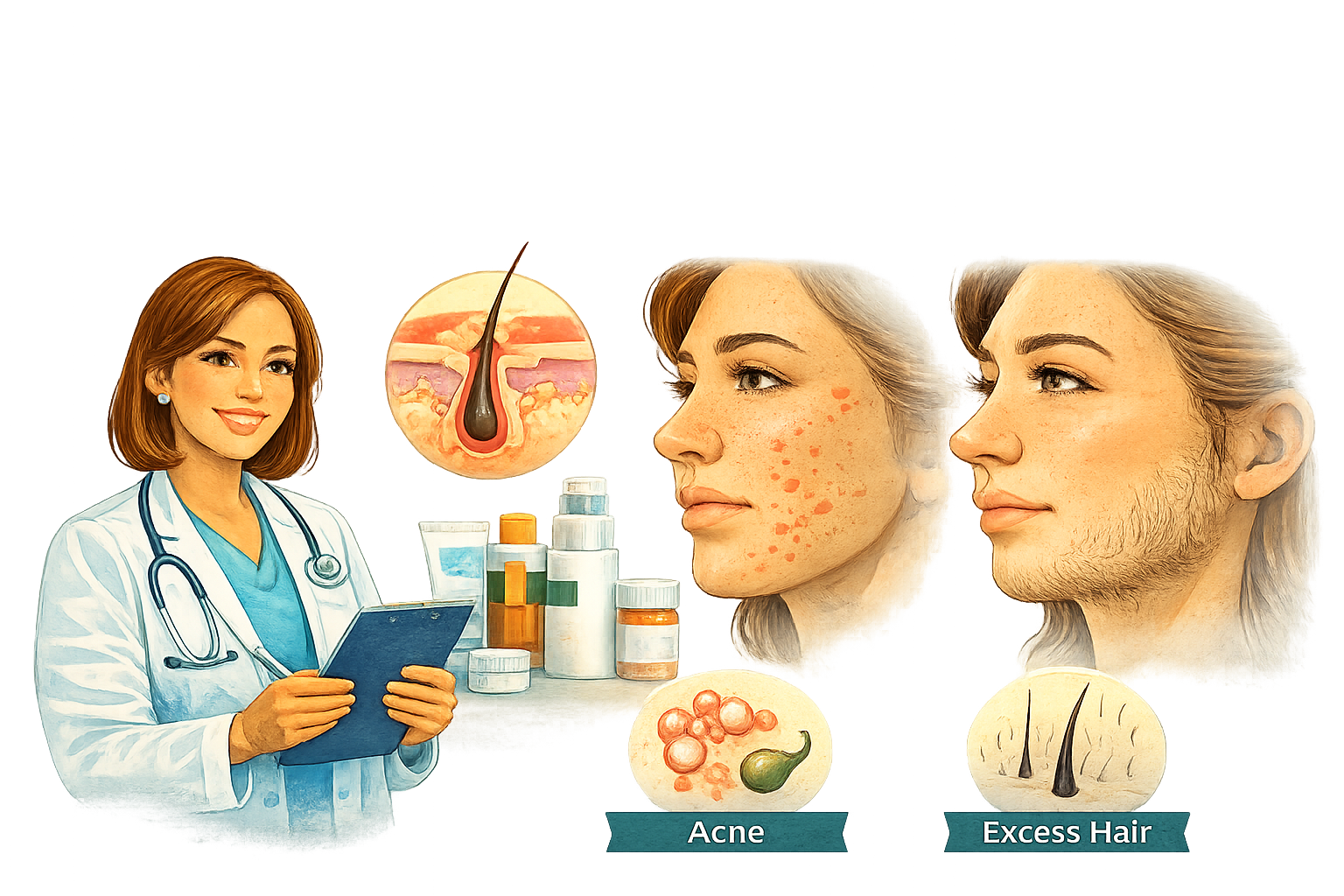
Many PCOS symptoms are visible on the skin and scalp.
How a dermatologist helps with PCOS:
Treating hormonal acne
Managing excess facial or body hair (hirsutism)
Addressing scalp hair thinning or hair loss
Treating dark skin patches linked to insulin resistance
When to see a dermatologist:
If acne, hair growth, or hair loss is persistent or affecting your confidence.
Registered Dietitian: Nutrition for PCOS Management
How a dietitian helps with PCOS:
Nutrition is one of the most powerful tools for managing PCOS symptoms.
Creating insulin-friendly meal plans
Supporting sustainable weight management (if needed)
Reducing inflammation through nutrition
Improving energy, blood sugar, and hormone balance
When to see a dietitian:
If you’re overwhelmed by PCOS diet advice or want a personalized, realistic approach to eating.

Mental Health Professional: Supporting Emotional Well-Being
PCOS is associated with higher rates of anxiety, depression, and burnout.
How mental health support helps with PCOS:
Managing anxiety and depression
Addressing emotional eating or body image concerns
Developing stress-management strategies
Coping with chronic illness challenges
When to seek support:
Any time PCOS affects your mental or emotional health—support is not optional, it’s essential.
Fertility Specialist: PCOS and Trying to Conceive
Not everyone with PCOS will need fertility treatment, but help is available.
How fertility specialists help with PCOS:
Tracking and supporting ovulation
Evaluating fertility health
Planning pregnancy with PCOS
Offering evidence-based fertility treatments
When to see one:
If you’re trying to conceive and not ovulating regularly or haven’t had success after several months.
Do You Need All These Doctors for PCOS?
Not necessarily. PCOS looks different for everyone.
Some people manage well with:
A gynecologist and primary care physician
Others benefit from a full care team that includes:
An endocrinologist
A dietitian
A dermatologist
Mental health support
The Bottom Line
PCOS is not just a reproductive condition—it’s a whole-body hormonal and metabolic disorder. The right medical team can help you manage symptoms, reduce long-term risks, and improve quality of life.
You deserve care that looks at the whole picture, not just one symptom at a time.


